 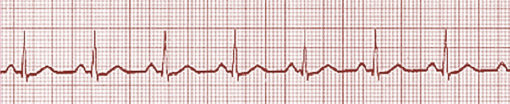
Each case of PEA is unique and the rhythm seen on the monitor will therefore differ from case to case. Organised electrical activity, often bradycardia (slower than normal heart rate). Potential causes must be sought and treated, including hypoxia, hyper/hypothermia, hypovolemia, hyper/hypokalaemia, pulmonary/cardiac embolus, tension pneumothorax, cardiac tamponade, toxins, thrombus, acidosis and ventricular rupture. It exists when there is a coordinated electrical rhythm (this includes a range of rhythms) without a detectable cardiac output. It may also be termed Electromechanical Dissociation (EMD). In a patient with a pacemaker, pacing spikes may be visible on the ECG strip. Rapid initiation of CPR and ALS measures is vital.Īsystole appears as a nearly flat line (except for those changes caused by chest compressions). The patient is pulseless and non-responsive. It is the absence of myocardial electrical activity and therefore produces no cardiac output. These non-shockable rhythms are asystole and pulseless electrical activity (PEA). The cardiac rhythms that do not require treatment with a DC shock are termed “NonShockable” rhythms. Heart rate: Ventricular rate of 100 bpm or above.Īdrenaline + CPR 2min NON SHOCKABLE RHYTHMS Rhythm: Regular or slightly irregular ventricular rhythm Alternatively it may be sustained, becoming symptomatic and causing unconsciousness, loss of cardiac output and death. 
It can occur in short bursts causing few or no symptoms. PVTs are extra heartbeats that disrupt the regular heart rhythm. It is defined as t hree or more premature ventricular contractions (PVCs) in a row, with a rate above 100 bpm. Heart rate: indeterminate Ventricular Tachycardia (VT) Left untreated VF invariably leads to ventricular standstill and death. The uncoordinated ventricular muscle quivers, therefore there is no effective cardiac output. It produces no effective myocardial contraction. It is commonly called VF (or V- Fib), an immediately life threatening condition. SHOCKABLE RHYTHMS Ventricular Fibrillation (VF) Start giving drugs after the third shock!.Attempt/verify: airway and oxygen, intravenous and intraosseous access.Check electrodes, paddle position and contact.The shock will immediately be followed by CPR 30:2 for 2 minutes without evaluating the rhythm or central pulse ! During CPR: Specificity for recognition of shockable rhythm close to 100%.Remove high flow oxygen from the defibrillation zone.Wipe any fluid from the patient's chest.Charge only with paddles on casualty's chest.Must be assumed by the person who applies electrical shocks.Biphasic shocks have higher success rate for ventricular fibrillation and pulseless ventricular tachycardia. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
